The Real Reasons You Are Not Sleeping Well

Do you know that perfectly rested feeling you get after a good night’s sleep? Have you noticed in contrast how awful you feel after a terrible night’s sleep? How about after multiple nights of terrible sleep? Adequate rest and sleep are paramount to your good health and, at the core, to basic survival.
Sleep Quality Matters
The quality of your sleep affects your attention span, your cognitive acuity and even your mood. That means that your ability to think clearly, regulate your emotions, and find joy in life is directly linked to how well you are sleeping at night.
And it’s not only your brain that’s affected, your body has many functions that rely on you getting regular deep sleep on a physiological level. Inadequate sleep can interrupt detoxing functions, disrupt hormones and contribute to a roster of health problems.

Sleep Quantity Matters Too – How Many Hours Do You Sleep?
Research has taught us that the average person needs a minimum of seven hours of quality sleep per night for their physiological functions and brain to function optimally, and that needs to be happening on a regular basis. It has also shown us that not everyone is getting nearly that amount of sleep, and many people don’t realize there is a huge connection between their sleep patterns and their health.
Modern Life is Creating Sleep Deficits
Why does this happen? Why are so many people unaware of their accumulating sleep deficits? Modern work demands, the increasing rarity of work/life balance, and the emergence of ‘toxic productivity’’ often celebrate our ability to get much done on little sleep. We are expected to do more on less rest, and sometimes that is to the detriment of our physical and physiological health.
Despite this, there is much you can do to improve the quality of your sleep and your health.
Why Am I Not Sleeping Properly?
While having a poor night’s sleep isn’t fun for anyone, it generally isn’t a reason for concern. We all experience it from time to time and our bodies are usually able to bounce back the following day after a decent night’s sleep. Not sleeping well does become an issue, however, if waking up tired every morning becomes the norm.
Insomnia
Insomnia is characterized by the inability to attain a good night’s sleep despite having the opportunity and environment to do so, with negative next-day consequences. In short, you sleep poorly, wake up tired or exhausted, and your next day is miserable because you don’t have the capacity to navigate it well. Insomnia is the most common sleep disorder, affecting approximately one-third of all adults.
Insomnia can take several forms:
- A high-sugar snack is eaten (candy bar, pastry, sweet cereal)
- Blood sugar levels rise fast, causing the pancreas to send out an emergency flood of insulin to move that glucose out of the blood and into the muscles.
- Blood glucose drops fast due to the flood of insulin, making you feel hungry again, with a particular craving for a sweet treat .
- You reach for another high-sugar snack to feed the craving, inadvertently starting the roller coaster ride all over again.
- High insulin inhibits melatonin production.
- You have chronic adrenal dysfunction leading to high evening cortisol levels.
- High cortisol levels inhibit anti-duretic hormone that can lead to needing to urinate throughout the night, disrupting sleep.
- You stay on your devices within an hour of bedtime (even two hours before can be disruptive) which raises cortisol and lowers melatonin.
- Doing high energy exercise within 3-4 hours before bedtime. (Notice how this affects you individually)
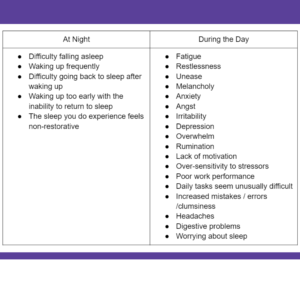
Insomnia Symptoms
You know you are experiencing insomnia when you experience any combination of the following:
Underlying Reasons You May Be Suffering From Insomnia
Stress
Despite insomnia being rather common, what causes it can differ greatly from person to person. Several factors can trigger it, with stress being one of the most common causes of insomnia whether it comes from a specific incident or ongoing stressors such as grief or work-related issues.
Poor sleep hygiene is a common problem, meaning, for example, not getting off of devices and screens (Television included) within 1-2 hours before bed-time. Also included:
-
- Exercising too close to bedtime or having high intensity lighting on in the home at night after dark.
- Having stressful conversations before bed-time.
- Having the last meal and liquids should be consumed 2-3 hours before bed-time.
- Avoiding caffeine after 2pm is recommended for good sleep hygiene..
Trauma
Physical and/or physiological trauma caused by one or a series of events can cause chronic insomnia despite feeling as though you have moved past it. Sometimes a past traumatic experience affects us more deeply than previously thought and needs to be addressed by getting the right professional help.
Health Issues
Chronic pain, nightly sleep apnea, regular allergies, and ongoing digestive issues or acid reflux can cause discomfort, making it hard to fall asleep and stay asleep – thereby disrupting your body’s natural sleep cycles. External issues such as disruptive noise, an uncomfortable mattress or pillow, invasive light through the window or from electronics, and temperature fluctuations can contribute to the same difficulties in falling and staying asleep. Certain medication side effects may also be factors, such as antihypertensives, hormonal medications, respiratory medications
Hormones
As women go through perimenopause, estrogen, progesterone, and testosterone all drop which can cause well-known symptoms such as hot flashes, mood changes and fatigue. These symptoms can mean interrupted or poor quality sleep. Estrogen can affect the body’s magnesium levels, a mineral that actively helps muscles relax. As estrogen levels drop, this can lead to restless, twitchy legs at night and even muscle cramps.
Men’s hormones are also affected by getting older, with lower testosterone levels being linked to similar sleep issues to those women face. When testosterone starts to drop, so do levels of feel-good neurotransmitters dopamine and serotonin, adding stress and anxiety into the mix.
Blood Glucose Levels
Fluctuating blood glucose levels and reduced insulin sensitivity become more common as we get older, and this is all the more marked in women going through the sudden hormonal disruptions associated with perimenopause. High blood sugar levels can make you feel too warm or irritable and unsettled, leading to difficulty falling and staying asleep.
Alcohol disrupts liver function and disturbs sleep, particularly after menopause. It is important to check your blood glucose levels regularly as you mature in years, as the risk of developing diabetes increases. If you can’t fall asleep due to feeling hot and bothered after dinner, talk to your healthcare practitioner about a glucose test.
Top Ways To Improve Sleep
Whatever the reasons for your insomnia, there is a lot you can do to help bring back some balance to your body and regain a more regular, restful night’s sleep.
Good Sleep Habits
We recommend practicing good sleep hygiene to ensure lasting and restful sleep. Sleep hygiene is the accumulation of regular practices that promote great sleep where you wake up feeling refreshed every morning.
Adopt the following to get a good night’s sleep:
Bedtime Sleep Hygiene
-
- Create a relaxing nightly routine that works for your lifestyle and stick to it (i.e. a warm bath or relaxing music)
- Go to bed at the same time every night
- Keep your bedroom quiet, dark and cool
- No screen time for at least one hour before bed
- Go to sleep on an empty stomach
- Don’t “try” to sleep
Daytime Sleep Hygiene
-
- Wake up at the same time every day
- Avoid stimulants (caffeine, nicotine) after 2:00 pm
- Limit your alcohol intake
- Avoid taking naps longer than 20 minutes
- Refrain from using your bed and/or bedroom for activities such as reading, working, or watching TV
Daily Lifestyle Habits for Optimal Sleep
-
- Exercise – Enjoy a minimum of 30-minutes of moderate daily exercise
- Supplements – Recommended for short-term use only, you can talk to your healthcare practitioner about whether magnesium, valerian root, ashwagandha, 5-HTP (5-hydroxytryptophan) or melatonin are appropriate for you. It depends on your history.
- Guided imagery, mindfulness meditation, progressive muscle relaxation, and breathing exercises
- Journaling
- Acupressure & acupuncture
- Cognitive Behavioral Therapy (CBT) – CBT is effective for chronic insomnia or insomnia caused by trauma. Speak to your health practitioner to find out more.
- Balance your hormones – hormone imbalances are common culprits when it comes to the quality of your sleep, and the quality of your sleep affects your hormone balance. Working with an Integrative/Functional Medicine practitioner allows you to uncover what’s really going on through thorough laboratory testing, and find a plan that works best for you.
We Can Help
If you have given it your best effort and are still not getting the restful sleep you need, We can help. As an Integrative/Functional Medicine Physician, together we can analyze what’s keeping you up at night and create a lifestyle plan to help improve the quality of your sleeping and waking hours. Book an appointment with us, and together we can move forward.
To learn more and to schedule a Free Discovery Call Consultation, visit our website HERE
Here’s to Great Sleep!
Valencia Ray, MD
References
Buysse DJ. Insomnia. JAMA. 2013;309(7):706-716. doi:10.1001/jama.2013.193
Cirelli C, Tononi G. The Sleeping Brain. Cerebrum. 2017;2017:cer-07-17. Published 2017 May 1.
Kaur H, Spurling BC, Bollu PC. Chronic Insomnia. [Updated 2020 Nov 19]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-.
Watson NF, Badr MS, Belenky G, et al. Recommended amount of sleep for a healthy adult: a joint consensus statement of the American Academy of Sleep Medicine and Sleep Research Society. Sleep. 2015;38(6):843–844. doi: 10.5665/sleep.4716
Worley SL. The Extraordinary Importance of Sleep: The Detrimental Effects of Inadequate Sleep on Health and Public Safety Drive an Explosion of Sleep Research. P T. 2018;43(12):758-763.


